Non-24-hour sleep-wake syndrome

INTRODUCTION:
Non-24-hour sleep-wake syndrome (Non-24) is a chronic circadian rhythm sleep disorder, classified within Chapter VI, Diseases of the Nervous System, in the ICD-10. It can be defined as "a chronic steady pattern comprising one- to two-hour daily delays in sleep onset and wake times in an individual living in society"
The pattern of delay persists literally "around the clock", typically taking a few weeks to complete one cycle. People with Non-24 "resemble free-running, normal individuals living in a time-isolation facility with no external time cues"
OTHER TERMINOLOGIES:
§ Free running disorder (FRD)
§ Hypernychthemeral syndrome
§ Circadian rhythm sleep disorder – free-running type
§ Circadian rhythm sleep disorder – non-entrained type
§ Non-24-hour circadian rhythm disorder
§ Non-24-hour sleep-wake disorder
The disorder is an invisible disability and "is extremely debilitating in that it is incompatible with most social and professional obligations"
Non-24-hour sleep-wake syndrome (Non-24) is a chronic circadian rhythm sleep disorder, classified within Chapter VI, Diseases of the Nervous System, in the ICD-10. It can be defined as "a chronic steady pattern comprising one- to two-hour daily delays in sleep onset and wake times in an individual living in society"
The pattern of delay persists literally "around the clock", typically taking a few weeks to complete one cycle. People with Non-24 "resemble free-running, normal individuals living in a time-isolation facility with no external time cues"
OTHER TERMINOLOGIES:
§ Free running disorder (FRD)
§ Hypernychthemeral syndrome
§ Circadian rhythm sleep disorder – free-running type
§ Circadian rhythm sleep disorder – non-entrained type
§ Non-24-hour circadian rhythm disorder
§ Non-24-hour sleep-wake disorder
The disorder is an invisible disability and "is extremely debilitating in that it is incompatible with most social and professional obligations"

SYMPTOMS
Symptoms reported by patients living according to a 24-hour day include:
§ Cognitive dysfunction
§ Confusion
§ Diarrhea
§ Extreme nausea
§ Extreme fatigue
§ Hair loss
§ Headaches
§ Ideational apraxia
§ Ideomotor apraxia
§ Impaired balance
§ Joint pain
§ Kinetic apraxia
§ Limb apraxia
§ Loss of muscle coordination (ataxia)
§ Menstrual irregularities
§ Muscle pain
§ Suicidal thoughts
§ Verbal apraxia
§ Weight gain
Symptoms reported by patients living according to a 24-hour day include:
§ Cognitive dysfunction
§ Confusion
§ Diarrhea
§ Extreme nausea
§ Extreme fatigue
§ Hair loss
§ Headaches
§ Ideational apraxia
§ Ideomotor apraxia
§ Impaired balance
§ Joint pain
§ Kinetic apraxia
§ Limb apraxia
§ Loss of muscle coordination (ataxia)
§ Menstrual irregularities
§ Muscle pain
§ Suicidal thoughts
§ Verbal apraxia
§ Weight gain
CAUSES
The etiologic of Non-24 is unknown in sighted individuals. However, chronotherapy has been known to cause it. According to the American Academy of Sleep Medicine (AASM): "Patients with free-running (FRD) rhythms are thought to reflect a failure of entrainment"
TREATMENT:
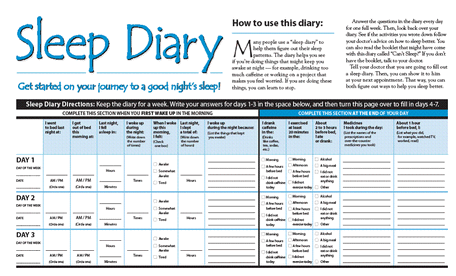
Common treatments for non-24-hour sleep-wake syndrome are similar to those for delayed sleep phase syndrome. They include light therapy with a full spectrum lamp giving—usually—10,000 lux, hypnotics and/or stimulants (to promote sleep and wakefulness, respectively) and melatonin supplements. In any case, a sleep diary should be kept to aid in evaluation of treatment
.Light therapy has been shown useful in treating DSPS; effects on patients with Non-24 are less clear. Melatonin administration has been shown to be effective for mild cases of Non-24, particularly among the blind. It often takes several treatments before any progress is noticed, and for many the treatments may only be marginally effective or not effective at all. In addition, the treatment is not a cure, and the condition may only be managed.
Bright light therapy combined with the use of melatonin as a chronobiotic (as per the PRC) may be the most effective treatment. However the timing of both is tricky and a lot of determination and experimentation is usually required.
The etiologic of Non-24 is unknown in sighted individuals. However, chronotherapy has been known to cause it. According to the American Academy of Sleep Medicine (AASM): "Patients with free-running (FRD) rhythms are thought to reflect a failure of entrainment"
TREATMENT:
Common treatments for non-24-hour sleep-wake syndrome are similar to those for delayed sleep phase syndrome. They include light therapy with a full spectrum lamp giving—usually—10,000 lux, hypnotics and/or stimulants (to promote sleep and wakefulness, respectively) and melatonin supplements. In any case, a sleep diary should be kept to aid in evaluation of treatment
.Light therapy has been shown useful in treating DSPS; effects on patients with Non-24 are less clear. Melatonin administration has been shown to be effective for mild cases of Non-24, particularly among the blind. It often takes several treatments before any progress is noticed, and for many the treatments may only be marginally effective or not effective at all. In addition, the treatment is not a cure, and the condition may only be managed.
Bright light therapy combined with the use of melatonin as a chronobiotic (as per the PRC) may be the most effective treatment. However the timing of both is tricky and a lot of determination and experimentation is usually required.
